Hand Foot and Mouth Disease: A Complete Guide for Parents and Caregivers
As a nurse practitioner, I understand the worry that comes when your child develops hand foot and mouth disease (HFMD). The distinctive rash and your little one’s discomfort can be distressing, especially when daycare requires a medical visit before return.
While there’s no magic cure for this viral infection, understanding what to expect and how to provide comfort can help both you and your child navigate this illness with confidence.

What Is Hand Foot and Mouth Disease?
Hand foot and mouth disease is a common viral infection primarily affecting infants and children under 5 years old, though older children and adults can also be affected.
The condition is most commonly caused by coxsackievirus A16 or enterovirus 71, both members of the enterovirus family. Despite its concerning name, HFMD is generally a mild, self-limiting illness that resolves on its own within 7-10 days.
Recognizing the Symptoms
The hallmark signs of HFMD typically appear 3-6 days after exposure and include:
Early symptoms (first 1-2 days):
- Fever (often the first sign)
- Sore throat
- General malaise and irritability
- Reduced appetite
- Runny nose
Characteristic rash (appears 1-2 days after fever):

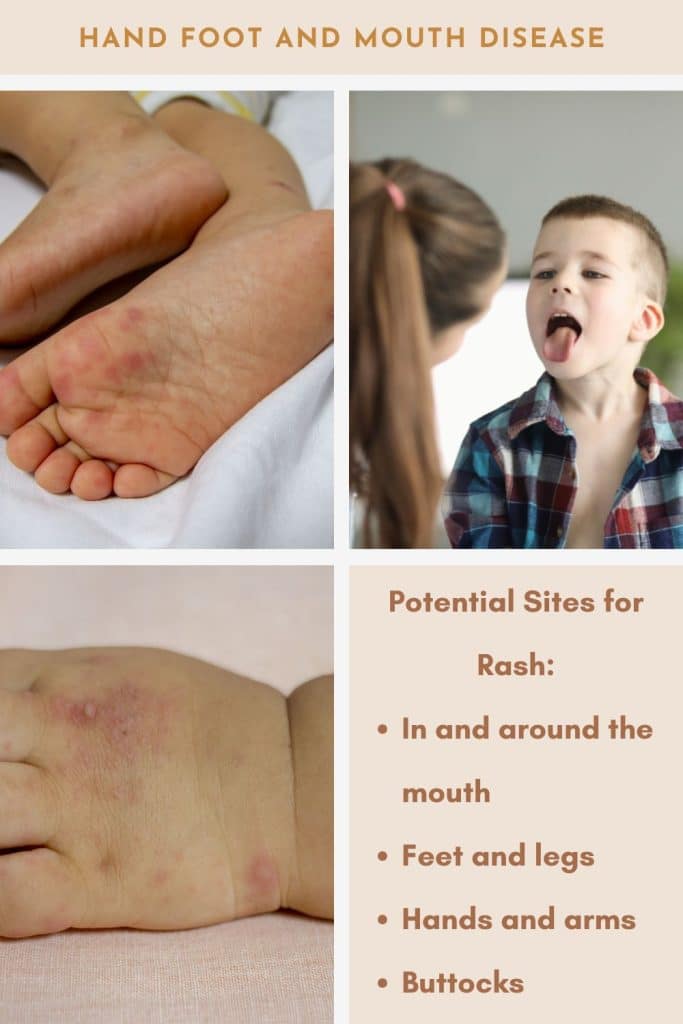
- Small, red spots or blisters on palms of hands
- Similar lesions on soles of feet
- Painful sores in the mouth, particularly on the tongue, gums, and inside of cheeks
- Sometimes a rash on buttocks, legs, or arms
The mouth sores are often the most uncomfortable symptom, making eating and drinking challenging for young children. These lesions start as small red spots and quickly develop into painful ulcers with gray centers and red borders.
Managing Symptoms at Home
Since Hand Foot and Mouth is viral, antibiotics are ineffective. Treatment focuses on comfort measures and preventing dehydration:
Pain and Fever Management
- Acetaminophen or ibuprofen according to age-appropriate dosing can help reduce fever and ease discomfort (dosing here)
- Never give aspirin to children due to the risk of Reye’s syndrome
Encouraging Fluid Intake
- Offer frequent small sips of cool liquids
- Avoid acidic beverages like orange juice or soda, which can irritate mouth sores
- Cold foods like popsicles, ice cream, or smoothies may provide relief
- For breastfeeding infants, continue nursing as tolerated—breast milk provides comfort and nutrition
Soothing Mouth Pain
- Cold liquids and soft foods reduce irritation
- Avoid spicy, salty, or acidic foods that can worsen mouth pain
- For older children, saltwater rinses (1/2 teaspoon salt in 1 cup warm water) may help
Skin Care
- Keep blisters clean and avoid picking at them
- Loose-fitting clothing prevents irritation of skin lesions
- Cool compresses can provide relief for uncomfortable areas
When to Seek Medical Care
While most cases of HFMD are mild, certain symptoms warrant professional evaluation:
Contact your healthcare provider if your child experiences:
- High fever (over 101.3°F/38.5°C) lasting more than 3 days
- Signs of dehydration (decreased urination, dry mouth, lethargy)
- Severe mouth pain preventing adequate fluid intake
- Difficulty breathing or swallowing
- Persistent vomiting
- Signs of secondary bacterial infection (increased redness, warmth, or pus)
Seek immediate medical attention for:
- Severe headache with neck stiffness
- Difficulty breathing or rapid breathing
- Chest pain
- Persistent high fever with altered mental status
A Surprising Late Complication: Nail Changes
One aspect of HFMD that often catches parents off guard is nail changes that can occur 4-6 weeks after the initial illness. This phenomenon, called onychomadesis, involves the temporary loss or shedding of fingernails and toenails. While alarming in appearance, this is a harmless late effect of certain strains of the virus.
What to expect:
- Nails may become loose and eventually fall off
- New nails will grow back normally over 3-4 months
- This occurs in approximately 10-15% of HFMD cases
- No treatment is necessary—simply keep nail beds clean and protected
If you notice nail changes weeks after your child’s recovery, remember this is a known consequence of the virus and not a sign of ongoing illness or poor healing.
Preventing Spread
HFMD is highly contagious, particularly during the first week of illness. The virus spreads through:
- Respiratory droplets (coughing, sneezing)
- Contact with fluid from blisters
- Contaminated surfaces
- Fecal-oral route (especially in diaper-changing situations)
Prevention strategies include:
- Frequent handwashing with soap and water for at least 20 seconds
- Disinfecting commonly touched surfaces
- Avoiding close contact with infected individuals
- Not sharing utensils, cups, or personal items
- Proper diaper disposal and changing hygiene

Children can return to daycare once fever-free for 24 hours and feeling well enough to participate in activities, even if some skin lesions remain.
Supporting Your Child Through Recovery
Recovery from HFMD is typically straightforward, but the discomfort can be significant for young children. Remember that:
- This illness will resolve on its own with supportive care
- Your child’s immune system is building protection against this specific strain
- Comfort measures are often more effective than you might expect
- Most children bounce back quickly once the acute phase passes
Final Thoughts
Hand, foot, and mouth disease, while uncomfortable and concerning for parents, is a common childhood illness that generally resolves without complications. Your role as a caregiver focuses on providing comfort, ensuring adequate hydration, and monitoring for signs that require medical attention. Trust your instincts—you know your child best.
While daycare policies requiring medical clearance can feel frustrating when you know there’s no specific treatment, these visits provide an opportunity to confirm the diagnosis, discuss comfort measures, and address any concerns about your child’s recovery.
Remember, experiencing HFMD is part of building your child’s immune system. With patience, appropriate supportive care, and close monitoring, most children recover completely and return to their normal, energetic selves within a week to ten days.
For more information, check the CDC’s website for more evidence based content: https://www.cdc.gov/hand-foot-mouth/about/index.html
This information is for educational purposes only and should not replace professional medical advice. Always consult with your healthcare provider for specific concerns about your child’s health.
